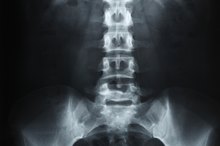
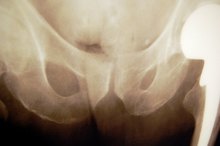
Symptoms of Thoracic Spine Pain
The thoracic spine is also called upper back, middle back or mid-back. Symptoms of thoracic pain affect the middle 12 vertebrae, known as T1 to T12. It is different in structure and function that the cervical spine, which is the neck or the lumbar spine which is the lower back. The thoracic spine gives stability and protection to the internal organs in the chest area.
Thoracic Disc Herniation
Depending on which disc is herniated, there are different symptoms. Some people with disc herniation may have no symptoms of thoracic pain at all. The most common causes of thoracic disc herniation are because of degeneration due to normal wear and tear and trauma, such as a car accident, fall or blow to the upper back.
A symptom of thoracic spine pain could be caused by a herniated disc in the upper back. It may be accompanied by pain that radiates down the back or numbness. Other symptoms are balance difficulties, problems walking, weakness, bowel or bladder dysfunction. Central disc protrusion could lead to paralysis from the waist down.
Thoracic Arthritis
Symptoms of Thoracic Spine Problems
Learn More
According to the Southern California Orthopedic and Musculoskeletal Associates, approximately 80 percent of people over the age of 55 in the United States will be affected by arthritis. Arthritis can affect any part of the spine.
General symptoms of thoracic pain caused by arthritis include: tenderness or numbness if there is nerve entrapment; the feeling or sound of bone crunching; limited range of motion; and pain or tenderness in the shoulders, hips, knees or heels.
Adult Kyphosis
Symptoms of thoracic pain can be caused by adult kyphosis. The word "kyphosis" means a type of curve in the spine. In the thoracic spine there is normally a slight curve, but if the curve is more than 40 to 45 degrees it is classified as a spinal abnormality. Kyphosis occurs commonly in the thoracic spine.
The four factors that can cause kyphosis are osteoporosis, congenital spine problems that affect development, the effects of medical treatment, surgery and traumatic injury. Symptoms of thoracic pain from adult kyphosis can vary from mild to severe. Some of the symptoms that may be felt are, weakness in the lower extremities, difficulty breathing due to the curvature of the thoracic spine and pain.
Thoracic Compression Fractures
Mild Lumbar Scoliosis Symptoms
Learn More
A common cause of thoracic compression fractures is from osteoporosis. Two other causes are trauma such a a car accident, a fall or any trauma to the spine that involves blunt force. Symptoms of thoracic spine pain cause by fractures are severe pain made worse by movement, weakness, numbness, tingling and bowel or bladder dysfunction.
Scheuermanns Disease
A cause of thoracic spine pain that affects teenagers is called Scheuermanns disease. If left untreated, it will cause rounded shoulders and poor posture. Symptoms include pain which is a deep ache rather than sharp, stabbing pain, and massaging the area will bring some relief for a short time.
Related Articles
References
Resources
Writer Bio
Marie Louise is passionate about her writing, bringing personal knowledge and experience on Complex Regional Pain Syndrome, chronic pain conditions, parenting, research, alternative medicine and animals. Her work appears on several different websites.